|
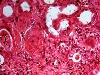
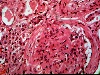
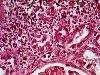
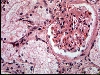
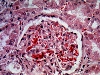
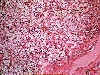
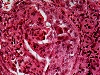
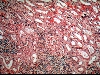
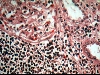
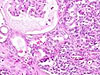
General and Systemic Histopathology, C601&C602 Renal Diseases Renal disease, and especially renal failure, can produce some of the most confusing and bewildering clinical symptoms of any organ system we will study. Because the kidney is involved with so many regulatory functions, presenting symptoms may vary from anemia to mental confusion or even pericarditis. But even though the symptomatology may vary dramatically, we will see there are a few common denominators. Renal disease is in large part a replay of microvascular disease. We will see time and again conditions that impact the functioning of capillary size blood vessels will be the principal causes of renal damage. Antigen-antibody complex diseases, such as lupus erythematosus and post streptococcal syndromes will serve as our models for auto-immune injury. Diabetes will weigh heavily as a major cause in many aspects of kidney pathology. Remember that for all practical purposes, diabetes becomes a small vessel disease. The consequences of diabetes lead to damage of the glomeruli, interstitial tissue and even the tubular epithelium. It should come as no surprise that diabetic renal disease is the leading cause of renal failure in the United States. Considering infectious diseases, the kidney and lower urinary tract will show us the problem of "opportunistic" infections. In most cases the microbial organisms causing infection of the urinary system come from our own body's normal flora. Living in their place, the bacteria of our GI system provide us vitamin K and creates a local environment hostile to many potential pathogens. But out of the normal habitat these same bacteria can produce life threatening infections. Finally, neoplastic disease
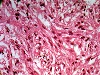
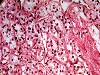
of the urinary system is almost in a class by itself. We will see varied
histological appearances of renal cell carcinomas as well as widely
varying clinical presentations. But even given the wide latitude of
clinical presentations and histological patterns of the tumors, if you know
the basics of the physiology of of the kidney you'll be able to puzzle your
way through most situations.
Previous Laboratory | Next Laboratory | Table of Contents
Copyright 1998, the Trustees of Indiana University
|